Cases Study

▋ Introduction
Since Hidalgo first successfully utilized the fibular free flap for mandibular reconstruction in 1989, this technique has become the gold standard for treating extensive mandibular defects following tumor resection.
With continuous advancements in Virtual Surgical Planning and 3D-printed surgical guides, the application of FFF in repairing mandibular defects has expanded significantly. By integrating modern digital implant dentistry, functional mandibular reconstruction using FFF can effectively restore a patient’s facial aesthetics and occlusal relationship.
However, a major limitation of the single-barrel fibular flap is its insufficient vertical height to accommodate standard implant lengths. Furthermore, the thick skin paddle often complicates impression-taking and increases the risk of peri-implantitis. In contrast, the double-barrel fibular flap effectively restores alveolar ridge height, maintains a favorable crown-to-root ratio, and enhances long-term biomechanical stability.
▋ Case Presentation
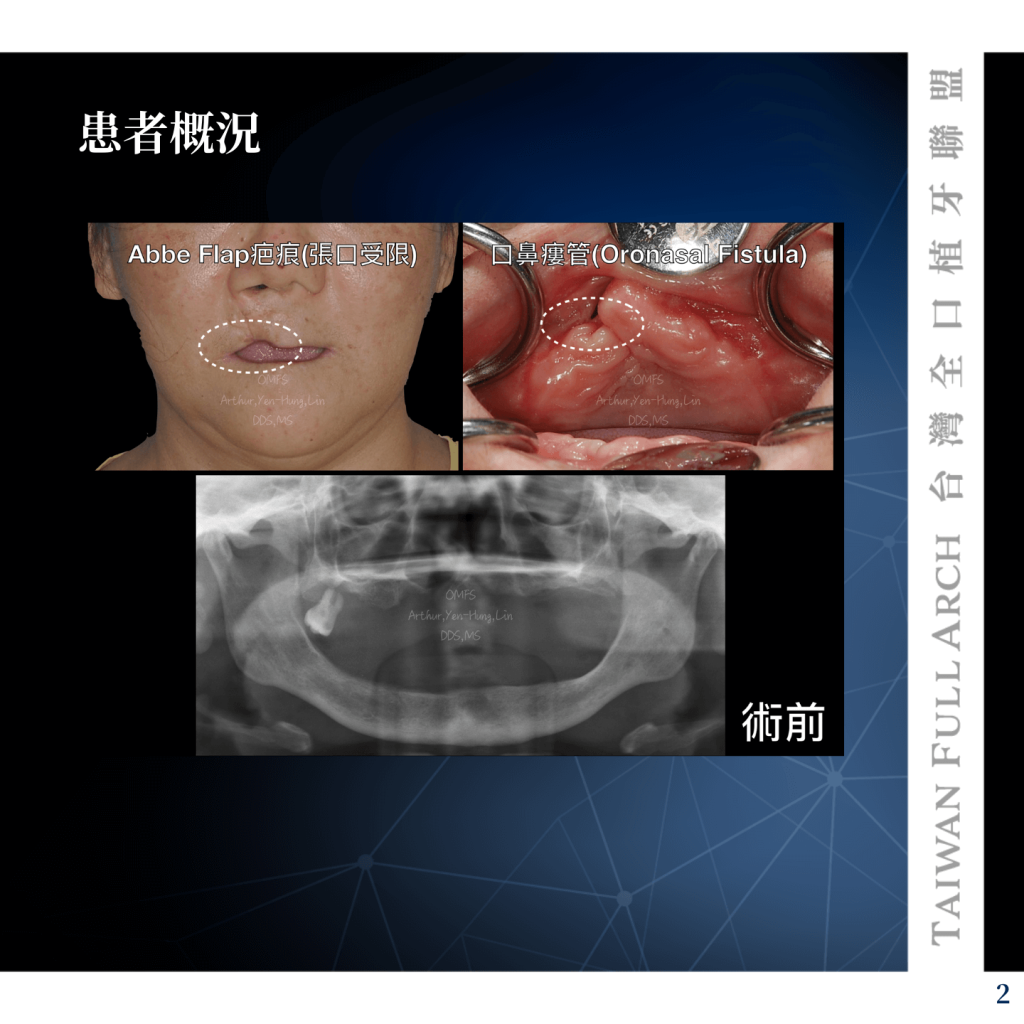
We present a 64-year-old male who previously underwent a mandibulectomy for ameloblastoma on the left side, reconstructed with a double-barrel fibular flap. One year post-surgery, with no signs of recurrence, he was referred by a prosthodontist for implant evaluation. We utilized the All-on-4 concept to restore his occlusal function.
▋ All-on-4 Implant Treatment Planning
Four NobelSpeedy Groovy implants (4.0 x 20mm) were planned at sites #31, #33, #34, and #36. Multi-unit Abutments (MUAs) were utilized to optimize the prosthetic screw access holes.
In flap-reconstructed cases, implant placement is often restricted by the underlying fibular bone geometry, leading to prosthetic challenges. MUAs are essential in these scenarios to compensate for implant angulation and simplify the restorative workflow. Additionally, a common complication is the development of hyperplastic granulation tissue at the skin-implant interface due to excessive flap thickness, which hinders oral hygiene and predisposes the patient to peri-implant disease.
▋ Soft Tissue Considerations for Peri-implant Health
A 2018 long-term study by Gerardo Pellegrino et al. analyzed surviving implants over 5 and 10 years, revealing:
A 14.8% prevalence of peri-implantitis and 20.3% for mucositis.
Patients lacking connective tissue or skin grafts had a higher risk of peri-implantitis (18.2%) compared to those who received grafts (9.5%), with an odds ratio of 1.5.
This underscores the critical importance of peri-implant soft tissue stability in flap-reconstructed patients.
▋ Flap Thinning and Prosthetic Phase
Due to excessive flap thickness prior to final prosthesis fabrication, a flap thinning (debulking) surgery was performed.
Because the double-barrel flap is inherently thinner than a single-barrel flap, we only required minor thinning. We utilized a 3D-printed custom guide to compress the flap relative to the implant positions, combined with a circummandibular wiring technique to secure the soft tissue. The guide was removed three weeks post-operation once the tissue stabilized, and the patient was referred back for the final prosthesis.
▋ Final Prosthesis Delivery and Follow-up
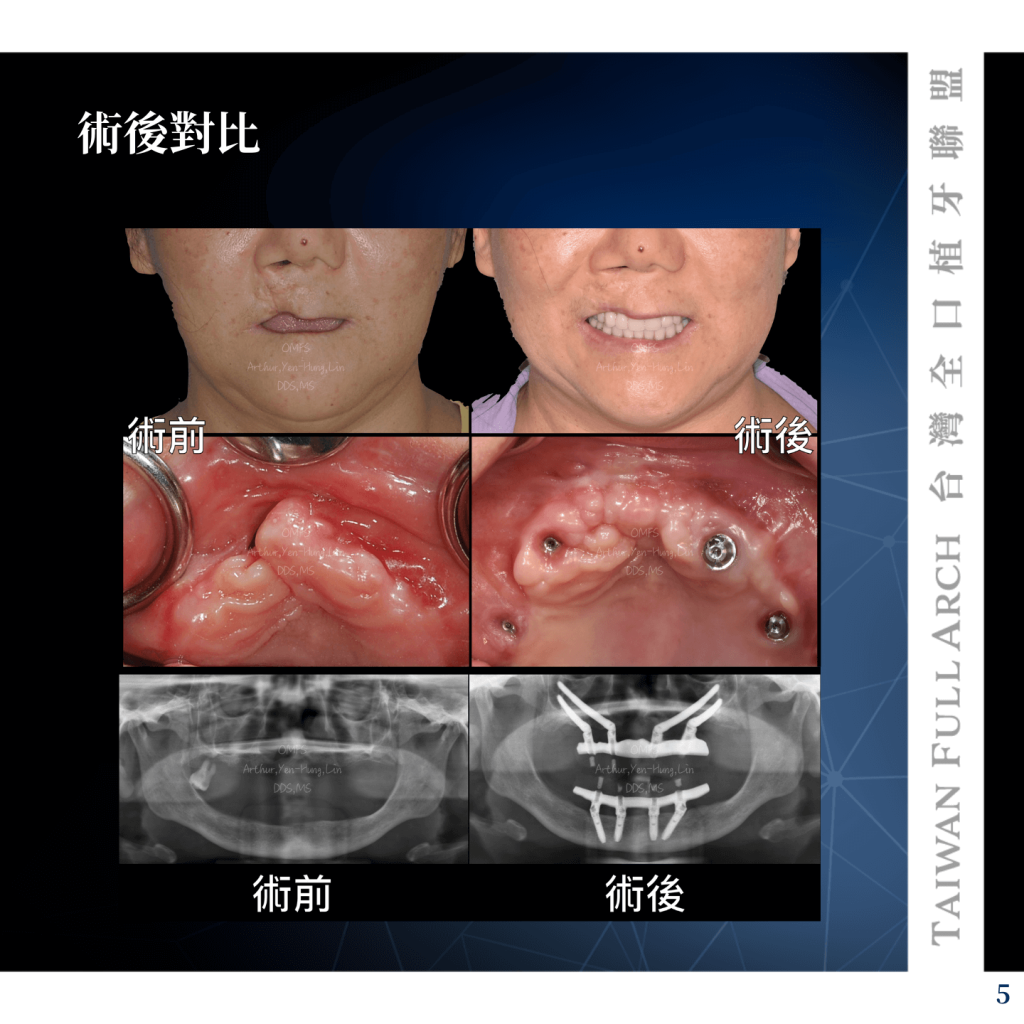
Following the delivery of the fixed prosthesis, the peri-implant soft tissue remained stable. Utilizing the All-on-4 concept makes maintenance significantly easier than traditional fixed bridges. The MUAs serve as a stable interface, and the screw-retained design allows the clinician to remove the prosthesis for professional cleaning if the patient is unable to maintain adequate oral hygiene.
▋ Conclusion
For patients undergoing mandibular reconstruction with fibula flaps, the All-on-4 concept is an excellent choice for functional recovery. It utilizes MUAs to overcome anatomical limitations and facilitates easier hygiene maintenance.
However, clinicians must recognize that the soft tissue surrounding these implants is skin flap tissue, which differs from native oral mucosa. Meticulous attention to soft tissue stability is paramount to preventing peri-implantitis and ensuring long-term implant success.